Provide Customers with Personalized Solutions
to Laser Applications
Provide Customers with Personalized Solutions to Laser Applications
GXF series femtosecond laser developed by INNU Laser has high average power up to 100W@1MHz for 1030nm. Higher peak power and excellent pulse energy makes it ideal to be applied in the material processing fields which needs higher precision. GXF series femtosecond laser can work under strict environment with low noise.






As the fourth generation of picosecond laser, the latest GXP series picosecond laser has high working efficiency with high output power, narrow pulse width and high peak power. More intelligent functions of remote data monitoring and diagnosis and laser self-protection are added, making it possible for maintenance on site. GXP series picosecond laser adopts new control system which is operated by INNGU OS 2.5 version software and supports BURST waveform editing, random trigger of POD pulse edges, PSO synchronous pulse output and management of constant single pulse energy.
Besides, it has ultra high power stability because of patented technology of independent seed source(50000 hours lifetime) and technology of intelligent zone divided amplifier management and multichannel thermostatic control.






Compared with nanosecond laser and picosecond laser, GXF series subnanosecond shows its excellent balance on high working efficiency and high precision on processing materials. The pulse width of GXF series subnanosecond laser is adjustable and ranges from 500ps to 20ns. GXF IR subnanosecond laser is especially designed for the application of 1mm-8mm thickness glass cutting.






INNGU nanosecond laser can be divided into 4 series: Grace X series, GS series, GP series and Pulse series. Compared to old version of Pulse series, Grace X series and GS series laser have integrated design without control box and compact structure. INNGU GP series 532nm water jet guided laser can be used for the cutting of extreme hard materials like diamond. INNGU 3W/5W UV nanosecond laser is widely used for 3D printing and marking on materials like plastic, glass, ceramic and etc. INNGU nanosecond laser can be operated by INNGU software of INNGU OS 2.0 version and controlled by RS232 or GATE/TTL/PWM externally.






INNGU provides customization for YAG and YLF laser as well as non-standard wavelength laser such as 1342nm IR laser, 527nm green laser and 266nm UV laser. Moreover, the customization of multi wavelength(dual or triple wavelength) laser is also offered. For all customized laser, necessary parameters are needed and it must be better for more detailed requirements.






Service and Support
Suzhou Inngu Laser, as a high-technology laser enterprise integrated with R&D, manufacturing, and selling, provides customized services for YAG and YLF laser, special wavelength laser and multi wavelength laser. Local after-sales service is also supported in some regions because INNGU laser has agents in some countries.
We are keen on the concept of Technological Innovation, Win-Win Cooperation, Integrity and Efficiency and First Rate Service to sincerely serve each customer. In addition, we intend to make a contribution to the development of laser high technology with all our counterparts.




Solutions
As the professional manufacturer of ultra DPSS laser source, INNGU LASER provides solutions in various fields such as industry, scientific research, medical treatment, solar energy and etc.

Suzhou Inngu Laser Technology Co., Ltd.
Suzhou Inngu Laser Technology Co., Ltd. is a national high-technology enterprise integrated with R&D, manufacturing, and selling. Over 40 patents have been granted, as well as honors like National High Technology Enterprise, Jiangsu Science and Technology SEMS, Jiangsu Private Technology Enterprise, Science and Technology Leading Talents in Suzhou Industry Park since it was established in 2013. INNGU Laser has a first-rank international technical research center, a hundred class ultra clean laboratory and workshop, and an advanced R&D team consisting of professional doctors and master talents in optical, electronic, software, and mechanical fields.
The femtosecond, picosecond, subnanosecond and nanosecond lasers produced by INNGU Laser are mostly used for applications like PCB precision cutting, cell phone manufacturing, semiconductor and glass cutting, 3D laser printing, solar cells, etc. We are keen on the concepts of Technological Innovation, Win-Win Cooperation, Integrity and Efficiency and First Rate Service to sincerely serve each customer. In addition, we are intended to make contributions to the development of laser high technology with all counterparts.
News
Laser technique could pave way toward therapies for alcohol addiction
Using laser light to temporarily inactivate a specific neuronal population, a team of researchers at The Scripps Research Institute (La Jolla, CA) have found th……
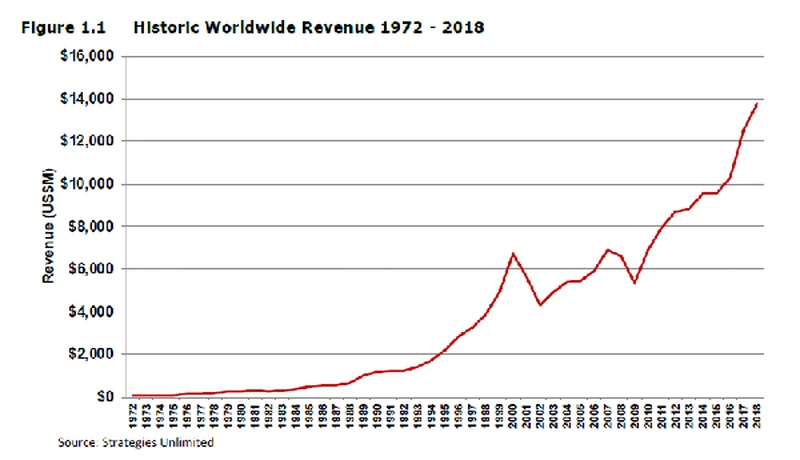
2019 Market for Lasers report now available from SU and Laser Markets Research
The 2019 worldwide laser market forecast report is now available for executive planning as the photonics industry prepares for 2020….
Aliens Might Shoot Lasers at Black Holes to Travel the Galaxy
An astronomer at Columbia University has a new guess about how hypothetical alien civilizations might be invisibly navigating our galaxy: Firing lasers at binar……